


| 1. | Prevent and/or delay the onset of diabetes among Members at increased risk due to their SMI and/or the addition of an antipsychotic medication, and |
| 2. | Manage and coordinate care for Members already diagnosed with diabetes and substance use disorders. |
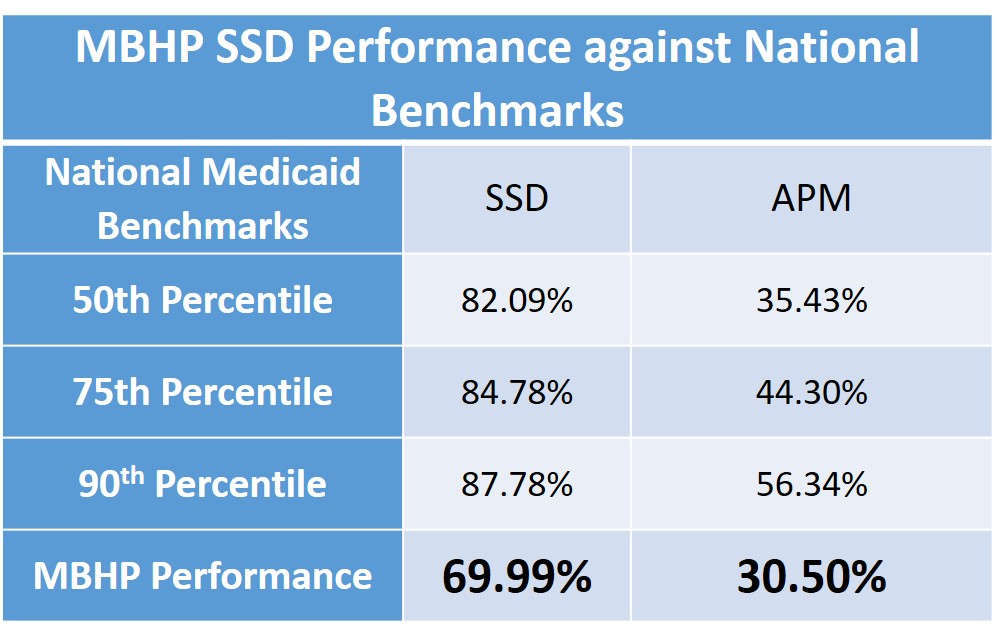
| 1. | Diabetes Screening for Members Taking Antipsychotic Medications for Bipolar Disorder or Schizophrenia (SSD): The percentage of Members 18 years of age and older who have been screened for diabetes after diagnosis with schizophrenia or bipolar disorder and prescription for an antipsychotic medication in the past year |
| 2. | Metabolic Monitoring for Children and Adolescents Taking Antipsychotic Medications (APM): The percentage of Members 1–17 years of age who have had two or more antipsychotic prescriptions filled and at least one metabolic test for blood glucose HbA1c and at least one test for low-density lipoprotein cholesterol (LCL-C) or total cholesterol each year |
 |
 |
 | |
| 1. | Inform providers on the importance of having Members diagnosed with serious mental illness screened for diabetes; |
| 2. | Promote coordinated care efforts through a team-based approach to better support Members in receiving the appropriate follow-up care and treatment; and |
| 3. | Identify opportunities and innovative strategies for increasing screening and metabolic monitoring across different levels of care. |